Why Does Psoriasis Keep Coming Back? Understanding Recurrent Psoriasis and Effective Management Strategies
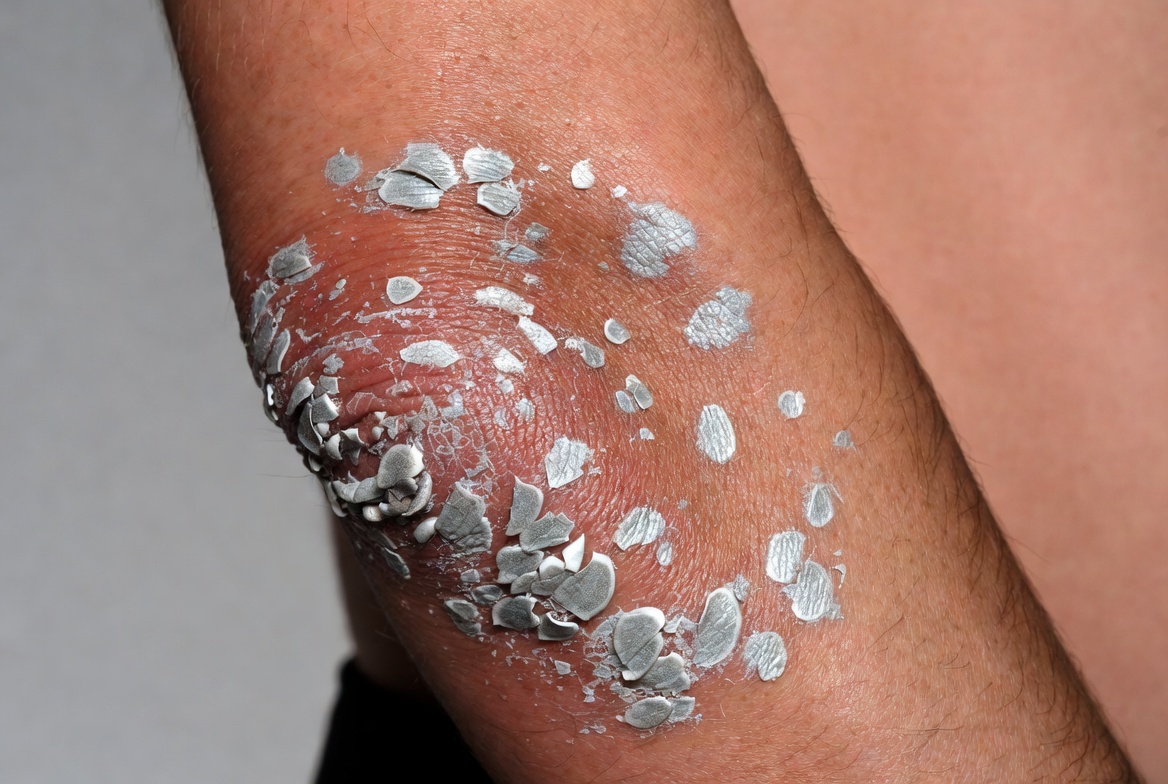
Psoriasis is a common chronic autoimmune skin condition that affects millions of people worldwide. It causes red, inflamed patches of skin covered with silvery-white scales, often appearing on the elbows, knees, scalp, and lower back. Many patients experience periods when symptoms improve or even clear completely—only for the condition to return weeks, months, or years later. This recurring nature is one of the most frustrating aspects of psoriasis. In this article, we explain why psoriasis keeps coming back and outline practical steps to manage it more effectively.
What Is Psoriasis?
Psoriasis occurs when the immune system mistakenly attacks healthy skin cells. This triggers an overproduction of skin cells—up to 10 times faster than normal—leading to the buildup of thick, scaly plaques. While it primarily affects the skin, it is a systemic condition that can also impact joints (psoriatic arthritis) and overall health. Genetics play a major role; certain genes increase susceptibility, but the disease often requires an environmental “trigger” to activate.
Why Psoriasis Is Chronic and Keeps Recurring: There Is No Permanent Cure (Yet)
Psoriasis is not a curable condition in the traditional sense. Even when the skin clears, the underlying immune dysfunction remains. Scientific research shows that “resident memory T cells” stay in previously affected skin areas. These cells act like a hidden “memory” of the disease and can rapidly reactivate inflammation when triggered.
Because of this persistent immune memory, psoriasis tends to recur at the same sites. New treatments (including advanced biologics and oral medications approved as of 2026) can achieve long remissions, but they typically require ongoing management rather than a one-time cure.
Common Triggers That Cause Psoriasis Flare-Ups
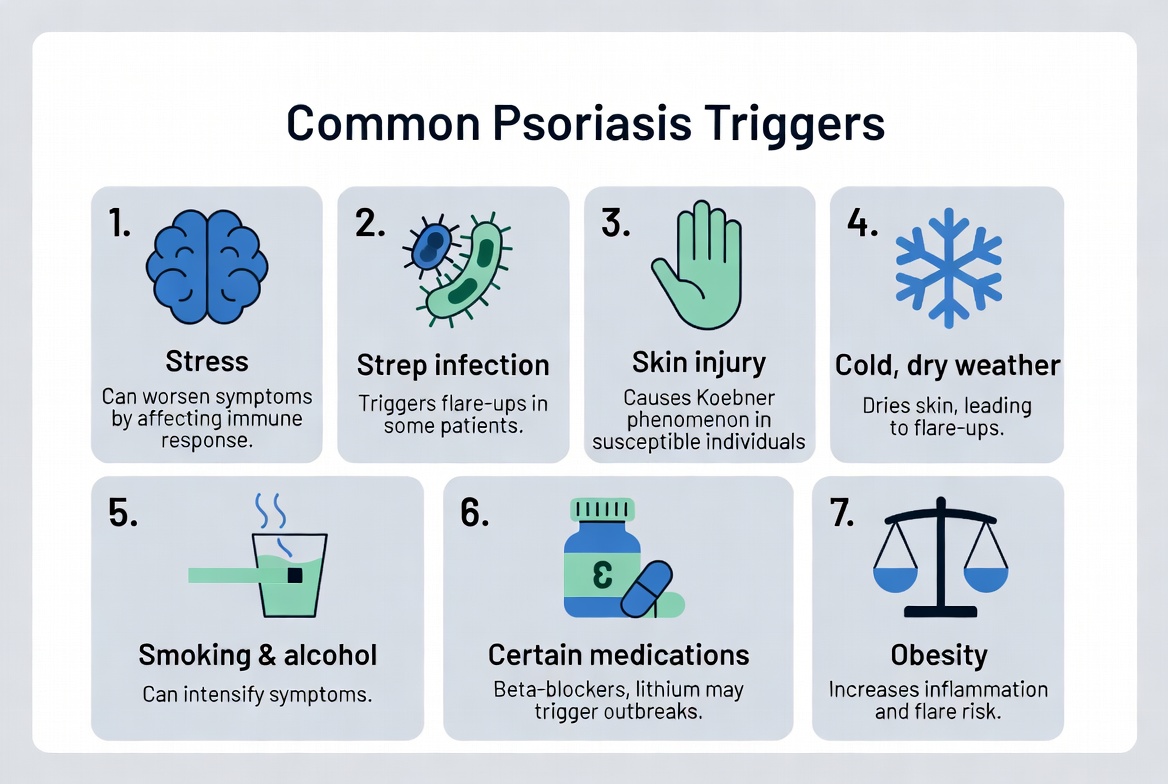
Flare-ups don’t happen randomly. Specific factors can awaken the dormant immune response. The most common triggers include:
- Stress: Emotional or physical stress releases inflammatory chemicals that worsen symptoms. Psoriasis itself can create a stress cycle.
- Infections: Especially strep throat or other respiratory infections, which often trigger guttate psoriasis in younger people.
- Skin injury (Koebner phenomenon): Cuts, scratches, bug bites, or even sunburns can cause new plaques to form at the injury site.
- Cold, dry weather: Low humidity and winter conditions dry out the skin and provoke flares.
- Smoking and heavy alcohol use: Both are strongly linked to more severe and frequent flares.
- Certain medications: Beta-blockers, lithium, antimalarials, and sudden withdrawal of oral steroids can trigger or worsen psoriasis.
- Obesity and lifestyle factors: Excess weight increases systemic inflammation.
Triggers vary from person to person. Keeping a symptom journal helps identify your personal ones.
How to Reduce Recurrence and Manage Psoriasis Long-Term
While you cannot eliminate psoriasis completely, you can significantly reduce flare frequency and severity with these evidence-based strategies:
- Follow a consistent treatment plan – Work with a dermatologist. Options include topical creams, phototherapy, oral medications, and biologics. Stopping treatment too early is a leading cause of quick relapse.
- Identify and avoid your triggers – Track stress, infections, and skin injuries. Use stress-reduction techniques like meditation, yoga, or regular exercise.
- Moisturize daily – Apply fragrance-free emollients immediately after bathing to lock in moisture and protect the skin barrier.
- Adopt healthy lifestyle habits – Maintain a healthy weight, quit smoking, limit alcohol, and eat an anti-inflammatory diet rich in fruits, vegetables, and omega-3s.
- Protect your skin – Avoid trauma, use sunscreen, and dress appropriately for cold weather.
Many patients achieve clear or nearly clear skin for extended periods with modern therapies and good self-care.
When to See a Doctor
If your psoriasis is spreading, becoming painful, or affecting your quality of life, consult a board-certified dermatologist. Newer treatments introduced in 2025–2026 (such as targeted oral peptides and advanced biologics) offer better long-term control than ever before. Early intervention can prevent complications like psoriatic arthritis.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. It is not a substitute for professional diagnosis or treatment. Please consult your dermatologist before making any healthcare decisions. We are not responsible for any damages arising from the use of this information

(1).jpg)