Understanding the Causes of Eczema (Atopic Dermatitis): A Medical Overview
Eczema, medically known as atopic dermatitis, is a chronic, inflammatory skin condition characterized by dry, itchy, and inflamed skin. It affects millions worldwide, often beginning in infancy or early childhood, though it can persist or develop at any age. While the exact etiology remains complex and multifactorial, current medical understanding points to an interplay between genetic predisposition, skin barrier dysfunction, immune dysregulation, and environmental triggers.
This article explores the primary causes based on evidence from leading dermatological and immunological research.
1. Genetic Factors
Genetics play a central role in the development of atopic dermatitis. A strong family history of atopic conditions—such as eczema, asthma, or allergic rhinitis—increases risk significantly.
The most well-studied genetic contributor is loss-of-function mutations in the filaggrin (FLG) gene. Filaggrin is a key protein in the epidermis that helps form the skin’s natural moisturizing factor and maintains the integrity of the stratum corneum (the outermost layer of skin). Mutations, present in up to 30% of patients, lead to impaired skin barrier function, increased transepidermal water loss, and greater susceptibility to allergens and irritants.
Key Highlight: Individuals with filaggrin mutations are also at higher risk for ichthyosis vulgaris, allergic sensitization, and the “atopic march” (progression to asthma and hay fever).
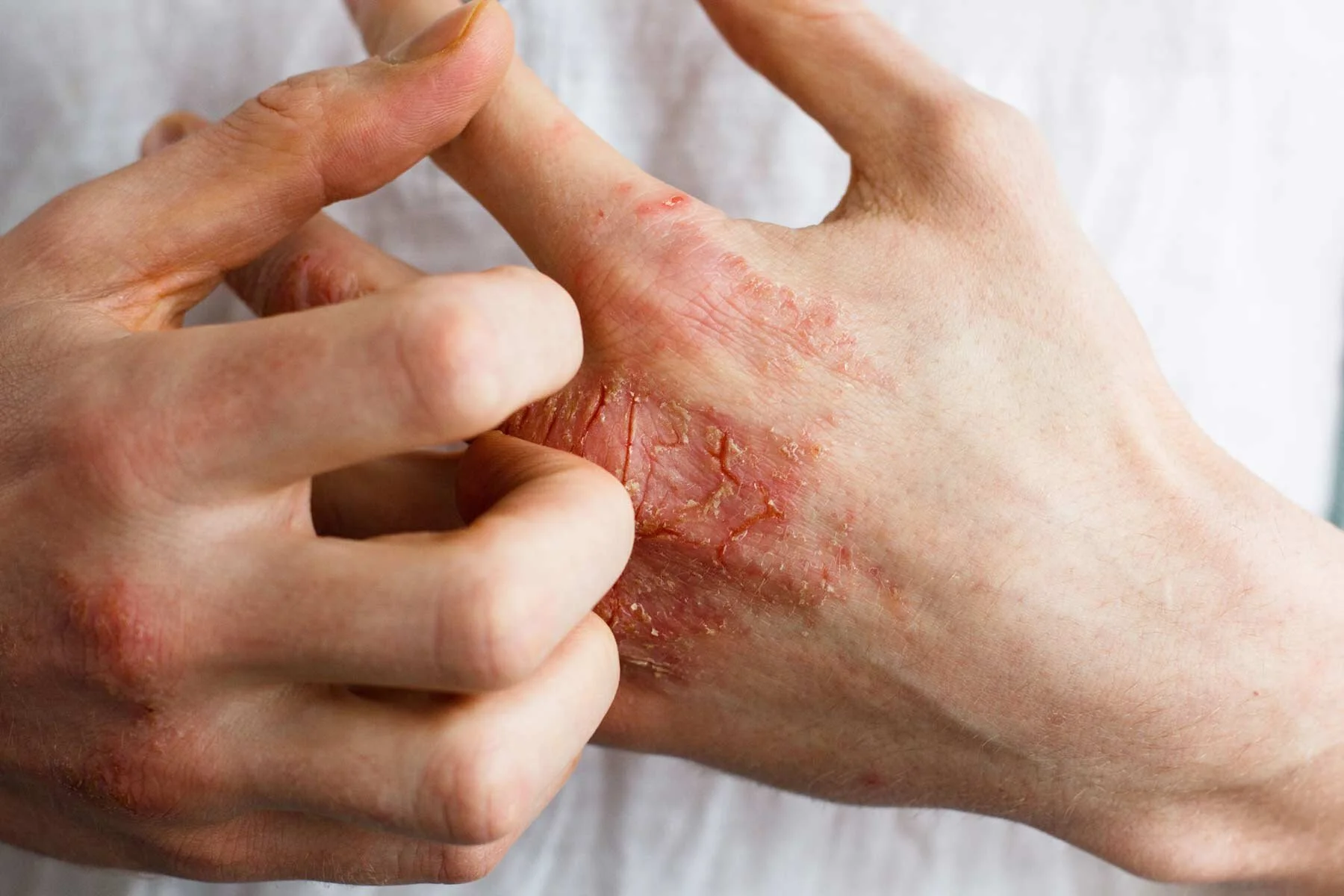
Clinical appearance of atopic dermatitis on the hands (images above). Note the characteristic erythema, scaling, and fissuring.
2. Skin Barrier Dysfunction
A defective skin barrier is a hallmark of eczema. In healthy skin, the stratum corneum acts like a “brick wall” with corneocytes (bricks) held together by lipids and proteins (mortar). In eczema, this barrier is compromised, allowing moisture to escape and external substances (irritants, allergens, microbes) to penetrate.
This dysfunction can be both a cause and a consequence of inflammation, creating a vicious cycle of dryness, cracking, and further immune activation.
Key Highlight: Overgrowth of Staphylococcus aureus on the skin further disrupts the barrier and exacerbates inflammation by displacing beneficial bacteria.
3. Immune System Dysregulation
Atopic dermatitis involves an overactive immune response, particularly a skewed T-helper 2 (Th2) pathway. This leads to elevated production of cytokines such as IL-4, IL-13, and IL-31, which drive itch, inflammation, and further barrier breakdown.
Many patients also show elevated IgE levels and sensitization to environmental allergens, though not all eczema is purely “allergic.”
Key Highlight: Immune dysregulation explains why eczema often coexists with other atopic diseases and why biologic therapies targeting IL-4/IL-13 (e.g., dupilumab) are highly effective.
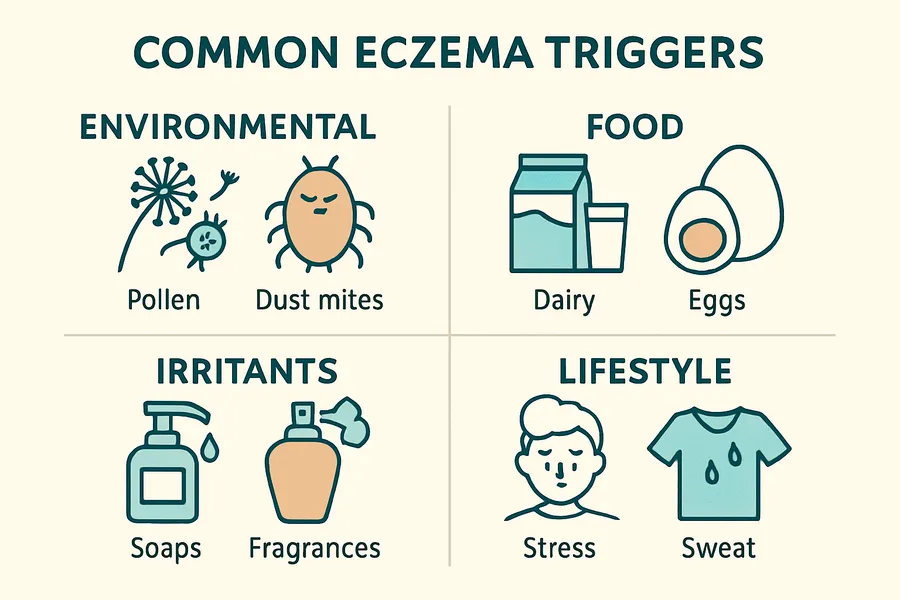
4. Environmental and Lifestyle Triggers
While genetics and barrier defects set the stage, environmental factors are major precipitants of flares. Common triggers include:
- Irritants: Soaps, detergents, fragrances, solvents, and wool clothing.
- Allergens: House dust mites, pollen, pet dander, and (in a subset of patients) certain foods (e.g., eggs, milk, peanuts).
- Climate and Pollution: Low humidity, extreme temperatures, air pollutants (soot, NO₂, SO₂), and tobacco smoke.
- Microbes and Stress: Bacterial or viral infections, sweating, and emotional stress.
Key Highlight: Identifying and avoiding personal triggers is one of the most effective non-pharmacologic strategies for long-term control.
5. Other Contributing Factors
- Microbiome imbalance: Reduced diversity of skin bacteria and dominance of pathogenic strains.
- Early-life exposures: Cesarean delivery, lack of breastfeeding, and urban living have been associated with higher risk in epidemiological studies.
- Age and ethnicity: Presentation and severity can vary across skin types and age groups.
Importantly, eczema is not caused by poor hygiene or contagious factors.
Conclusion and Clinical Takeaways
Atopic dermatitis arises from a complex interaction of genetic susceptibility, impaired skin barrier, immune hyperactivity, and environmental insults. Understanding these causes empowers patients and clinicians to implement targeted prevention and management strategies, including daily emollients, trigger avoidance, and advanced therapies when needed.
Important Medical Note: If you or your child experience persistent itchy rashes, consult a board-certified dermatologist or allergist for personalized diagnosis and treatment. Early intervention can prevent complications such as skin infections and the atopic march....
Disclaimer: This article is for educational purposes only and does not constitute medical advice. It is not a substitute for professional diagnosis or treatment. Please consult your dermatologist before making any healthcare decisions. We are not responsible for any damages arising from the use of this information

(1).jpg)

